The patient
A trauma alert was rolled into room 5 at the 'Port. A 45 year-old male, restrained driver in a roll-over, who had been ambulatory on EMS arrival. He was mildly intoxicated, denied any significant medical problems. His vitals were normal both prehospital and in the ED. (The trauma alert was due to mechanism, not his condition.)
His exam was notable for a rather large laceration to his scalp, with a correspondingly large blood clot at the head of the backboard.
 |
| "He probably smells my dog!" |
The bleeding was controlled, and the evaluation continued.
While we were getting the chest x-ray, however, we noted that his heart rate, which had intially been around 70-80, started slowing down. 60, 50, 40, down to the 30s!
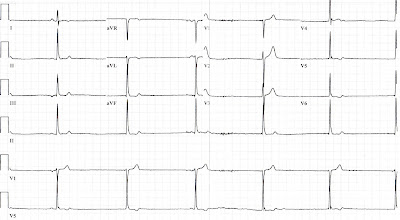
His blood pressure, which had also been normal, plunged down to a systolic BP of around 50 mmHg. His ECG showed this:
An old ECG was entirely normal. Interestingly, the patient, in a supine position the whole time, denied any symptoms whatsoever, and was moderately amused by our concern.
Discussion
So what happened to his heart?
Well, we should worry first about ischemia- or infarction-related bradycardia. An inferior MI is notorious for causing 1° and 2° AV blocks, most of which resolve on their own. These bradycardias manifest with a narrow QRS, since the block involves the AV node, but not the bundle of His, etc. They usually get better in a few days, on their own.
By contrast, anterior MIs may involve an infarct of part of the ventricular conduction pathways. The patient will have a wide QRS and a high-grade 2° or 3° AV block. These are bad, and need permanent pacemakers!
Although you should think of hyperkalemia when you see bradycardia, there was little else to suggest it. He denied any medications, so digoxin, beta-blockers, and calcium-channel blockers seemed unlikely, especially given how quickly the rhythm had developed after normal prehospital vital signs.
Perhsps I should be clearer about how the bleeding from the scalp was controlled. Since the wound was large, and the bleeding brisk, a number of staples were rapidly placed.
 |
| NOT an approved wound closure technique. (credit) |
Let's take a closer look at the ECG. Like I said before., he gradually slowed down to 34.
Sinus activity is almost extinguished - I can only find 2 P-waves, preceding beats #1 and #3. The QRS is narrow, suggesting a junctional rhythm, albeit much slower than you would expect (usual junctional rate is 40-60). You can't really call it complete heart block, since there is so little atrial activity; instead, it's just called AV dissociation.
Putting all this together, it appears he had a cardioinhibatory/reflex syncopal episode; i.e. he fainted. The placement of the staples likely triggered a strong vagal reflex, which inhibited both the sinus node (almost no P-waves) and the AV node (junctional bradycardia).
Fortunately he was already supine when it occurred!
 |
| Inappropriate stapling technique. |
He got atropine 0.5 mg IV, and a liter of NS on a pressure bag. His heart rate corrected quickly, coming up to about 80, but his blood pressure took a few more minutes to come up! He was admitted, and did not have any more bradycardic episodes.
Bottom line
No harm, no foul, as they say. But I do think we're going to be more enthusiastic about using lidocaine in the trauma bay, however!

Massive Head Wound Harry!!
ReplyDeleteNice example of "dissociation by default."
My question is if the Bradycardia and Hypotension would have self corrected even without the interventions?
ReplyDeleteMos def!
DeleteInterestingly, the squirt of atropine bumped up the heart rate, but didn't really do anything for the blood pressure. I was sort of laughing at myself as I asked for a pressure bag on the IV bag, since, given the context, it seemed pretty clear that this was going to work out either way. And it did.
Eh, I'm okay with "treating myself," or "treating the monitor" on occasion. Especially when the HR + SBP < 100.
As I've been known to say, "Sometimes it's important to resist the urge to just do something and stand there."
ReplyDeleteAs you mentioned, next time give more Lidocaine before stapling. An ounce of Lidocaine is worth a pound of Atropine. ;)
An ounce... I'm stealing that!
DeleteAnother guy stealing my material. Sheesh, who do you think you are, Ambulance Driver? ;)
DeleteI found out, that taking herbal treatment is the best to get rid of hpv as soon as i feel the symptoms of hpv is appearing, i took the healing process by contacting Dr onokun for natural treatment it works wonders, amazingly ever since I had the herbal treatment i have not feel these horrible disease anymore and my doc told me the virus is gone, i am glad i finally got cured out from this horrible disease. every hpv or herpes patients should also get in touch with this herbalist Dr to get ride of these disease forever his email address; dronokunherbalcure@gmail.com
ReplyDeleteI started on COPD Herbal treatment from Ultimate Health Home, the treatment worked incredibly for my lungs condition. I used the herbal treatment for almost 4 months, it reversed my COPD. My severe shortness of breath, dry cough, chest tightness gradually disappeared. Reach Ultimate Health Home via their website www.ultimatelifeclinic.com I can breath much better and It feels comfortable!
ReplyDeleteI really want to thank Dr Emu for saving my marriage. My wife really treated me badly and left home for almost 3 month this got me sick and confused. Then I told my friend about how my wife has changed towards me. Then she told me to contact Dr Emu that he will help me bring back my wife and change her back to a good woman. I never believed in all this but I gave it a try. Dr Emu casted a spell of return of love on her, and my wife came back home for forgiveness and today we are happy again. If you are going through any relationship stress or you want back your Ex or Divorce husband you can contact his whatsapp +2347012841542 or email emutemple@gmail.com website: Https://emutemple.wordpress.com/ Https://web.facebook.com/Emu-Temple-104891335203341
ReplyDelete