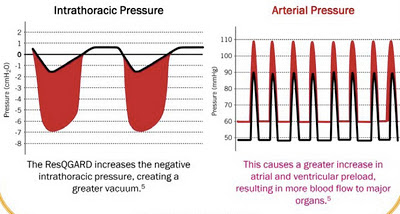
One development in EMS in the past few years has been the push in many states to get prehospital providers to carry and administer steroids to people with various forms of adrenal insufficiency. Unlike cardiac arrest, intubation, or cervical spine injury, there hasn't been a great deal of talk in the EMS blogs about this subject, so I was hoping to address that deficit!
First off, why should I care about adrenal insufficiency?
Well, one answer is that some one is going to make you care. Most likely, that someone will be the CARES Foundation. This group was started by the parents of a child with congenital adrenal hyperplasia (CAH) (relax if you aren't familiar with CAH - we don't see it very often in the ED!). Back in 2009, they started focusing on the role of EMS in treating children with CAH. If we take a look at this map of the United States that shows which states have EMS protocols for treating CAH crises:
We can see that the advocacy efforts of the CARES Foundation has been quite successful in changing protocols in the northeast part of the country, with one small exception - Connecticut!
The more astute readers will say - "Hey! Out of every 16,000 live births, only one will have classic CAH! That doesn't sound too common." Well, yeah, you're right. On the other hand, there are a lot of people out there in the world with adrenal insufficiency, and they can get into the same problems.
Sooo... What is CAH, adrenal insufficiency, and stuff like that?
Let me explain the two forms of adrenal insufficiency you'll deal with. This is a crazy-deep topic, but there will be basically two kinds of steroid problems you'll see.
- Little kids with a known diagnosis of CAH, and,
- Adults with a diagnosis of adrenal insufficiency who tell you that.
Let me give a very brief review of the physiology of adrenal problems. So, this gets complex fast, but there are some main points. Here's a picture of how steroids get made in the body.
- The hypothalamus makes CRH.
- When some of that CRH drifts by the pituitary, it makes some ACTH.
- In turn, the ACTH triggers the production of cortisol from the adrenal gland.
- Eventually, the elevated cortisol levels shut down (temporarily) the production of CRH and ACTH.
- When the cortisol levels settle down, the process is ready to go again!
Adults can a variety of different problems with their steroid-making process: Maybe the have Addison's disease, like a former president did. Maybe their adrenal glands eroded during an infection. Maybe they're taking mondo amounts of steroids to prevent transplant rejection, and their body has "forgotten" how to make it's own steroids now. These folks also are on chronic steroids.
 |
| Nope. Try again. |
Okay, it sounds like we have the problem solved then!
Er, almost. The problem is that the body regulates the ebb and flow of cortisol over a wide range of levels. For example, your morning level is about 10 times higher than your midnight level.
When you get sick, no one is quite clear what the right level should be. When kids get sick, parents are taught that their daily dose of pills should be significantly increased, and are given detailed instructions (PDF download) about when to, say, double or triple their usual dose.If things get real bad, they have a emergency steroid injection kit, and the parents have practiced how to draw up and give the shot.
Good, the parents are all over it. What's left for us?
Well, even fairly small kids can't hang around their parents all day, every day. They may get stuck with. well-meaning relatives, day-care, or even a lowly babysitter. While the parents may be up to speed on the the when and how of injected steroids, it's asking a bit much to expect 16 year-old sitter to do that too.
 |
| Not what she signed up for. |
Naturally, you know all about assessing acute adrenal insufficiency, right?
What do adrenal-insufficient people in a crisis look like?
First off, these people already have a history of chronic adrenal insufficiency. That begs the important question: What exam finding indicates a patient has chronic adrenal insufficiency?
 |
| Answer |
Next part in assessment is figuring out what else is gong on. Something had to trigger an episode of acute insufficiency; there are diverse causes, but all of them stress the body in some way. The general causes, though, are: Stopped steroids abruptly, fever/infection, a large trauma, vomiting. The New Hampshire protocols, for instance describe which patients to treat with specific therapy:
Patients will look shaky, gray, sweaty. The may be hypotensive and hypoglycemic as well.
The paramedic should look at the precipitating events, and treat those, whether it's a trauma, an asthma attack, a burn, a bad episode of gastroenteritis, or pneumonia. Second, they should address the symptoms of the episode: Zofran for vomiting, dextrose if they're hypoglycemic, IV fluids for hypotension. An EKG could show signs of hyperkalemia, and you should be ready to ask med control for calcium chloride.This is all stuff you should be doing now.
The specifc therapy for acute adrenal insufficiency is hydrocortisone, or Solu-Cortef:
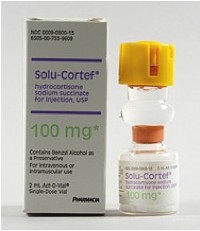 |
| Adult dose = 1 box, IM, IV, or IO. |
So, be ready for the change when it comes!